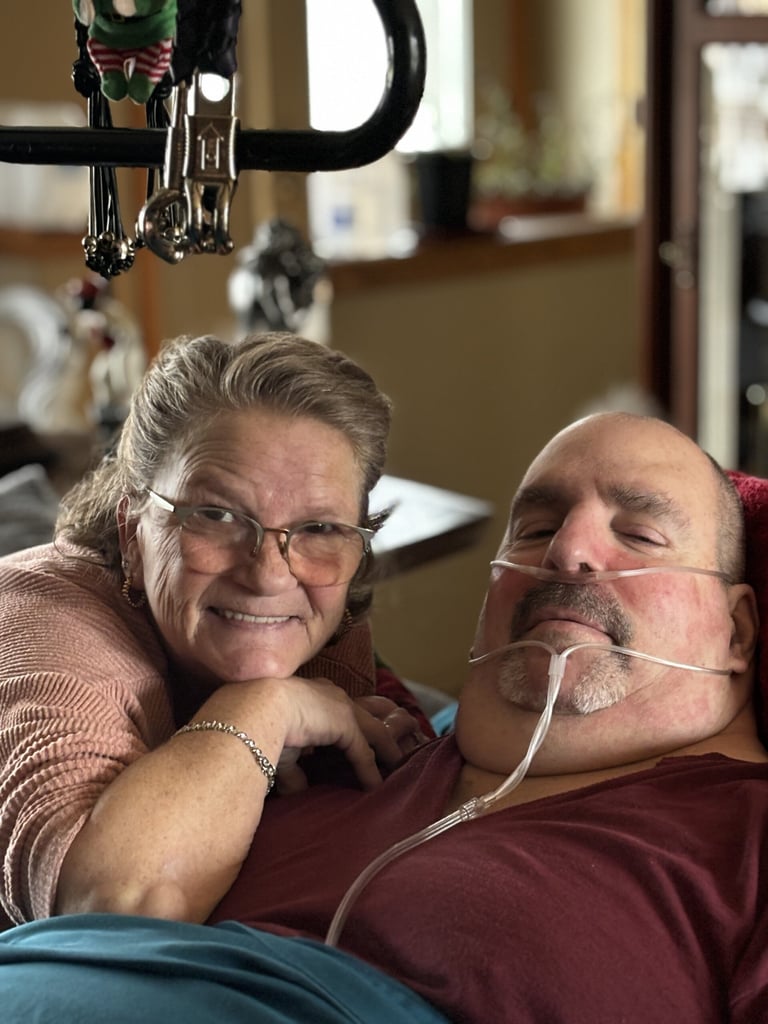
Find Peace of Mind with Personalized HospiceCare
We specialize in honoring and supporting your loved one as they enter the next phase of life. Our team of skilled professionals provides clinical expertise with dignity, respect, and understanding.
We welcome all who qualify for services. And as the only Des Moines metro hospice provider that is a 5-star member of We Honor Veterans, we are specially qualified to serve your military family.


Experience authentic support that feels like home.
WesleyLife has provided personalized end-of-life care to individuals throughout the Des Moines area since 2007. Our hospice at-home services are available 24 hours a day, seven days a week. We are honored to support clients and their families with comfort and encouragement.
“Mom was ready to go. I knew she wouldn’t have wanted to suffer, and WesleyLife Hospice made the process comfortable and as pleasant for her and for all of us as possible. In the end, Mom was at peace.”
Count on the expertise of clinical professionals.
Many people are surprised to find that hospice can provide a sense of relief, both to individuals facing the end of life and families who love them. Having sympathetic professionals on hand to assist with medical needs, pain management, and emotional well-being eases the burden and paves a path toward meaningful connections.
“My mama was blessed to have WesleyLife Hospice take care of her in her final days. They made it possible for her to pass in her own home. The compassion and care was outstanding. From the bottom of my heart, I will always be thankful they were a part of our lives. I would highly recommend this wonderful organization to family and friends.”

We salute those who have served.
WesleyLife Hospice is the only Des Moines metro hospice provider that is a 5-star partner of We Honor Veterans. Our affiliation with this national program allows us to:
- Understand veterans' unique end-of-life emotional needs
- Serve veterans in ways that honor their military experiences
- Provide customized care to families and other loved ones
We would be honored to serve your family.


Enjoy memories in life's next chapter.
Hospice is a beautiful, meaningful support system available to anyone experiencing end of life in their family. Help from WesleyLife Hospice means your family can focus on what’s important at this time: expressing feelings, showing love, and making memories.
“They took care of my mom through her illness and passing. Gentle, caring, and supportive, as well as knowledgeable and professional. So grateful for how they helped our family. ”
Lend a helping hand.

Interested in becoming a hospice volunteer?
By lending a hand with hospice, you can make a difference in the lives of deserving individuals and their loved ones.
We offer volunteer opportunities across Iowa during the daytime, evenings, or on weekends. Volunteers don't need any experience or medical background, and training is provided at no cost. You may choose to volunteer a couple of hours a month, a few hours a week, or more often.
In addition, we are always seeking volunteers with military experience to help with pinning ceremonies, veteran-to-veteran cafes, and more. Allowing those special vet-to-vet connections to form can result in more meaningful experiences for those we serve. If you served in the military and are curious about volunteering, please reach out to us so we can tell you more.
Clients and families share their stories.
Learn more about what it's really like to be part of a WesleyLife community or be served by our organization.

Find peace of mind during life's next chapter.
Give comfort, support, and dignity to the ones you love.
Explore hospice care at WesleyLife.
Hospice care encompasses a variety of specialized services designed to support a person’s well-being after being diagnosed with a life-limiting condition. The goal of hospice is not to cure or treat a person’s medical condition but to manage symptoms and provide as much comfort and enrichment as possible.
A person is eligible for hospice care when their doctor diagnoses them with a life-limiting condition with a prognosis of six months or less. If you’re not sure whether you or your loved one qualifies, consult with your medical team.
Very few clients pay for hospice services out of pocket. Typically, costs are covered by insurance, whether Medicare, Medicaid, or a private insurance policy. This includes all costs associated with hospice care, including nursing services, counseling, medical equipment, and more.
(Note that you may augment your or your loved one’s care at your own expense through at-home services.)
A doctor may recommend hospice care when their patient’s prognosis is six months or less, but it’s always up to individuals and families how they will proceed. It’s never too early to learn about hospice care so you’re prepared to make an informed decision when the time comes. Those who are eligible for hospice may consider calling hospice when:
- Their health is in serious decline.
- Their strongest desire is for comfort, not curative medical treatment.
- Family caregivers need professional support.
Consult with your medical team and loved ones as you determine the right time to engage end-of-life services.
Each client’s hospice care plan is tailored to their needs. Hospice care can include a variety of services, such as:
- Non-curative medical care
- Short-term inpatient care
- Medical equipment and supplies
- Home health aide and homemaker services
- Physical, speech, or occupational therapy
- Counseling services and spiritual support
WesleyLife families can also receive long-term bereavement services for loved ones through hospice care.
Some clients receive hospice care in a free-standing hospice center. However, generally speaking, hospice is not a place—it’s a service that can be delivered in a variety of settings. Most hospice clients receive care wherever they call home, whether that’s a senior living community, a family member’s home, or their personal residence.
Hospice care at home refers to hospice care services delivered in a home setting as opposed to a dedicated hospice facility. All WesleyLife hospice services are delivered to clients in the comfort of their own homes.
Hospice care and palliative care share similarities, but they are not interchangeable. Both forms of care focus on enhancing overall well-being and quality of life for someone with a serious illness. However, hospice care is reserved specifically for individuals with a prognosis of six months or less, whereas palliative care is open to anyone with an incurable condition.
The decision to receive hospice care can be a difficult one, but it often comes with a flood of relief for a person and their loved ones as they set aside the stress and effort involved in curative treatments and embrace more comfort-oriented care. Hospice can enrich a person’s final chapter by:
- Helping them manage symptoms and minimize discomfort.
- Supplying them with medical equipment needed to support their care.
- Allowing them to enjoy the comforts of home.
- Providing guidance to help them and their family navigate this stage of their health journey.
- Supporting their and their loved ones’ emotional and spiritual well-being.
In 2021, Medicare members who were enrolled in hospice spent an average of three months in the program. Families can choose to engage end-of-life services at different points in their health journey, so some patients may receive hospice care for just a matter of days, whereas others may receive care for months.
Choosing to receive hospice services sooner rather than later can be extremely beneficial for clients and their families. This choice could save you from paying out of pocket for specialized services and equipment such as hospital beds or shower chairs. Note that many individuals benefit from hospice care for more than six months, and a client can continue to receive hospice care should their condition progress slower than predicted.
The decision to receive hospice care marks a shift in your medical treatment as you discontinue curative measures and focus instead on palliative care.. However, you may still be able to see your regular doctor if you designate them as the attending medical professional overseeing your hospice care. Check with your hospice organization and insurance provider to determine whether this is an option for you and whether the cost will be covered.
Some clients find that the care they receive through hospice, while not curative, positively impacts their health. If a person’s health improves while on hospice care, they may choose to shift their focus back to curative treatment. Hospice clients are free to discontinue hospice care at any time if it’s no longer an appropriate fit for their needs. If they remain eligible or become eligible once again in the future, the client can reengage hospice care when they’re ready.
Hospice care is a valuable resource for both clients and their families. Hospice professionals and volunteers support families and caregivers in a variety of ways, including:
- Delivering personalized, skilled care, lessening the caregiving burden on families.
- Sharing information and answering questions to help families understand their loved one’s condition and needs.
- Remaining on-call at all times to provide information over the phone or in-person assistance when needed.
Providing emotional and spiritual support, including bereavement services to families for a year after their loved one’s passing.
Hospice care is not strictly focused on physical needs; it’s holistic care designed to support all aspects of a person’s well-being, including their spiritual and emotional needs. Some ways hospice meets these needs include:
- Social interaction with friendly team members
- Religious guidance and prayer from a chaplain
- Clinical counseling for hospice clients
- Bereavement services for family members
One of the benefits of hospice care at home is that families do not need to abide by visitation rules that may apply in a clinical setting. A hospice care team may make recommendations to support the client’s well-being, but it is ultimately up to the client and their loved ones to decide when and how they will spend time together.
In the event of your loved one’s passing, a hospice care nurse or other qualified professional will legally pronounce death and handle the next steps to arrange transportation for your loved one to the funeral home of your choosing. Navigating the death of a loved one can feel overwhelming, but your hospice care team will serve as a source of compassion and practical help during this difficult time.
Even if you’ve discontinued curative care, you may experience a medical emergency (such as a sudden increase in pain) that necessitates swift action. In these instances, you should not hesitate to call 911. However, you should also notify your hospice care team, which is available around the clock. If a hospice nurse is present, they may be able to manage the crisis without the need to leave your home. Speak with your hospice care team about what you should do in the event of a crisis so you’re prepared.
Didn't find an answer? We can help!

Join our mission.
Your donation can make a real difference to the thousands of people we serve. Please consider making a contribution to the WesleyLife Foundation.
Explore our latest blog posts.
Explore our latest posts to learn more about care options, considerations, and support.